Dozens of states across the country together gave more than $380 million in Medicaid funds to medical providers who were later caught defrauding the federally funded program, and in many cases, after years of pocketing payments, according to a Washington Examiner analysis of Medicaid spending data.
Some states continued to pay providers post-conviction, including a deceased doctor, or allowed banned providers to bypass federal restrictions by using other healthcare organizations to bill Medicaid for reimbursement on their behalf.
The findings, which came to light amid the Trump administration’s efforts to crack down on healthcare fraud, are based on recently released Health and Human Services records documenting provider-level Medicaid payments from January 2018 to December 2024, which the Washington Examiner cross-referenced with the agency’s list of “exclusions.”
HHS’s exclusions database blacklists individuals and entities that are actively banned, or “excluded,” from accessing federal healthcare dollars for a variety of offenses, largely fraud-related reasons.
Which states failed to catch fraudsters for years
Arizona, Ohio, Nevada, Kentucky, and New York were the five worst offenders that failed, for years, to catch these scheming service providers sooner before they eventually landed on the federal exclusions list, the Washington Examiner found.
Oversight officials in Arizona, which outpaced only Ohio with $95 million in Medicaid checks cut to now-convicted fraudsters, approved nearly $99 million in Medicaid payments to such scammers over that seven-year reporting period.
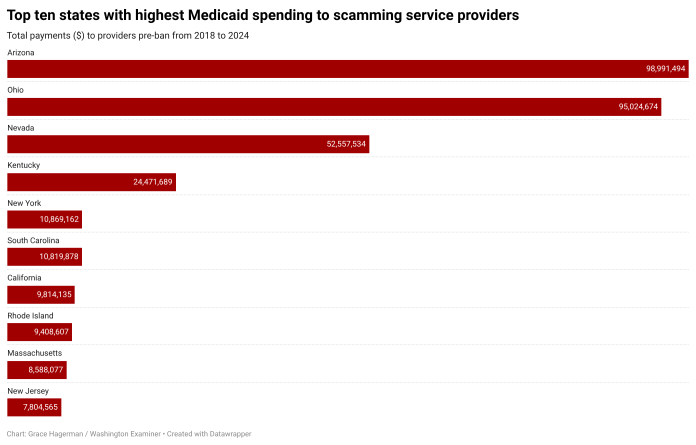
For example, Arizona paid James Demasi, the owner of New Life Wellness Center, a substance abuse treatment clinic with two facilities purportedly located in Phoenix and Flagstaff, more than $80.6 million in those allocations alone from 2021 to 2023.
Demasi pled guilty in 2024 to “ghost billing” for services that were never actually provided, engaging in fraudulent double-billing practices, and even charging Medicaid for the care of dead patients.
Up until his conviction, Demasi at one point had averaged about $8.7 million a month in Medicaid payments between the two clinic locations, both of which dumped patients at a dilapidated motel that served as transitional housing.
Residents reportedly lived in deplorable conditions at the since-shuttered recovery site, an unlicensed behavioral health center called the Thomas Suites Campus of Care, where there were reports of rampant drug dealing and no running water. A website for the halfway house advertised A.I.-generated images of tattooed people supposedly recovering from drug addiction.

In response to a Washington Examiner request for comment, Arizona’s state-level Medicaid agency, the Arizona Health Care Cost Containment System, noted that the $99 million in claims cited came before their exclusion dates.
Indeed, for example, a provider banned in 2025 for committing fraud was legally allowed to bill for services in 2024, when the fraud had not yet been caught. And a ban does not mean that all billing before the ban date was fraudulent.
When factoring in the exclusion date, the data shows that Arizona has not paid out any claims to providers once they were caught. State officials, after running all providers against claims in AHCCCS’s system, confirmed that the agency approved zero payments to providers after the date on which they were placed on the exclusions list.
AHCCCS found 303 instances of providers submitting attempted claims after their exclusion date, and each was appropriately denied, the department told the Washington Examiner.
“While there will always be fraud in healthcare,” the agency said, “under the leadership of the Hobbs Administration, the Medicaid behavioral health schemes that proliferated at AHCCCS under the prior administration have come to an end.”
According to AHCCCS, the schemes started during the previous administration of former Gov. Doug Ducey (R-AZ) but have since been “snuffed out” by the department.
An agency spokesperson said that AHCCCS, with Ducey’s successor, Gov. Katie Hobbs (D-AZ), at the helm, has become “a national leader in program integrity” by imposing an 18-month enrollment moratorium for certain provider types prone to fraud, requiring prior authorizations for covered services that were abused by bad actors, and implementing pre-payment review audits on specific claims to verify medical necessity, coding accuracy, and documentation validity.
In 2023, the U.S. Centers for Medicare & Medicaid Services told AHCCCS that Arizona is “the success story for identifying and responding to Medicaid fraud,” the spokesperson added.
Since then, 138 indictments have been issued from AHCCCS fraud referrals, with 46 indictments already resulting in convictions or guilty pleas.
States continued to dole out millions of Medicaid dollars to banned providers
Each state is responsible for regularly checking the exclusions list to ensure that state agencies administering Medicaid do not enroll or continue to disburse payments to excluded entities.
Providers prohibited from participating in the Medicaid program, however, have continued to collect at least $5.5 million in payments despite their publicly listed expulsion status on the HHS repository.
Of the most egregious examples of post-exclusion billing that the Washington Examiner identified in the datasets, one physician’s practice in Trion, Georgia, raked in over $271,000 in Medicaid claims after he was banned by the HHS inspector general’s office, doing so, in fact, for three years following the doctor’s death from a brief illness.
Dr. Gary Lee Smith, Sr., agreed to a 10-year ban starting in 2021, admitting that he submitted false Medicaid claims for the prescriptions of Schedule II controlled substances, which are highly addictive drugs considered dangerous and potentially lethal when ingested, such as cocaine, methamphetamine, oxycodone, and fentanyl.
Smith died that same year, according to an obituary. Smith’s practice, however, still billed Medicaid for hundreds of reimbursement claims in his name between 2021 and 2024.
His national provider identifier, a unique 10-digit identification number that every eligible entity uses to bill Medicaid for services rendered, has since been deactivated.

We Care Transportation, a non-emergency medical transport company operating out of a P.O. box in Overland Park, Kansas, was federally excluded in 2010 but accrued more than $4.4 million in Medicaid fee-for-service funds between 2018 and 2020.
As of 2025, the company’s NPI is still active, and its exclusion status has not been lifted.
In Minneapolis, Minnesota, a home healthcare agency named Twin Cities Care Services received $116,000 in reimbursements over just two months in 2024, even though the business was busted eight years earlier for Medicaid fraud. Twin Cities Care Services was convicted in 2016 of four counts of theft by false representation.
According to court documents, its owner, Somali businessman Abdulkarim Dahir, admitted that TCCS “always” billed the maximum number of hours allowed by the Minnesota Department of Human Services per patient visit, rather than the actual time staff spent, seemingly providing personal care assistance to Medicaid recipients.
On multiple occasions, TCCS overbilled for more than eight hours a day, even though no personal care supervisor worked more than eight hours a day.
HOW MINNESOTA’S SOMALI FRAUD INDUSTRIAL COMPLEX HAS STOLEN MILLIONS FROM MEDICAID
For four years, Dr. Mohamed Basel Aswad, a Syrian-born oncologist in the tiny town of Deming, New Mexico, took in a total of $674,000 in Medicaid claims from 2018 to 2022, despite being banned since 2016 due to a fraud-related conviction.
Aswad previously pled guilty to illegally introducing “misbranded” cancer drugs into interstate commerce, a federal crime. A prescription drug is considered “misbranded” if it is manufactured in a facility not registered with the Food and Drug Administration for commercial distribution within the U.S.
To cut down on the cost of chemotherapy and allegedly generate revenue for himself, Aswad had ordered an injectable drug approved for use in Turkey, but not the United States, from a foreign pharmaceutical company and then distributed the shipped product to his patients.
By importing the drug from abroad, via a 1-800 phone number, Aswad paid significantly less than he would have had he purchased an FDA-approved version of the label, yet he billed federal healthcare programs for the product’s full market price. According to disciplinary documents, Aswad was reimbursed approximately $1.3 million by Medicare, Medicaid, and TriCare for the medication’s purchase.
The New Mexico Medical Board ordered an immediate suspension of Aswad’s medical license, determining that he “posed a clear and immediate danger to the public health and safety” should he continue to practice medicine.
Aswad was also forbidden by the federal government from accepting Medicaid or Medicare reimbursements for a minimum of 13 years. But because of the area’s shortage of medical specialists, the New Mexico Human Services Department requested a waiver on his behalf that permitted him to resume practice and continue treating cancer patients as the only oncologist in all of Luna County, a remote rural region.
In spite of his criminal history, Aswad was accordingly allowed to treat Medicaid and Medicare patients in four other “medically underserved” New Mexico counties.
Aswad additionally contested HHS’s decision to bar him from seeking reimbursement for treating Medicaid and Medicare patients, who comprised about 95% of his clientele.
State human services officials agreed Aswad should “be allowed to participate as a Medicaid provider on a limited basis as the sole provider of essential and specialized cancer-fighting services in a rural/remote part of New Mexico,” an HSD spokeswoman told Albuquerque Journal at the time.
HEALTHCARE FRAUD HAS PROLIFERATED NATIONWIDE, HOUSE REPUBLICANS WARN
“It was determined that the imposition of exclusion [from seeking the federal reimbursement] would not be in the public interest” and instead be “a hardship for New Mexicans in the southwest region of the state who would have to make onerous arrangements for travel and treatment in other locations if not for Dr. Aswad’s availability and participation in Medicaid,” the spokeswoman said.
Medicare and Medicaid Services also approved the expansion of Aswad’s coverage area during the COVID-19 pandemic.
Aswad, while he was on federal probation, was given the government’s blessing to treat patients, allegedly underdosing a patient with colon cancer as part of an apparent scheme to profit from the prolonged treatment plan. That patient, James Hoag, then died.
A jury in 2021 ultimately found Aswad liable in a $2.3 million wrongful death lawsuit, which began as a medical malpractice case when Hoag was alive. Attorneys for Hoag alleged that Aswad administered “woefully lower” doses of chemotherapy and intentionally dragged out the typical six-month regimen by more than double the recommended duration in an attempt to pocket the proceeds.
“It was statistically likely that James would have beaten his cancer with proper treatment,” Hoag’s legal counsel argued at trial.
Aswad’s medical license is still active, according to the state’s license look-up.
Bypassing the ban: Backdoor billing schemes
A common tactic of Medicaid con artists who are otherwise not entitled to tap reimbursements themselves, whether because of a criminal conviction or because they are not registered Medicaid providers, is to have other certified individuals or organizations bill the government on their behalf.
Through these backdoor billing schemes, bad actors can bypass the screening process designed to prevent them from collecting reimbursements directly. In such arrangements, the parties typically split the payments, with the authorized entity completing the reimbursement paperwork and the ineligible provider ostensibly performing the services billed.
Sometimes a provider’s NPI is used without their knowledge or consent, a crime known as NPI theft that is commonly committed to facilitate Medicaid fraud.
“Medicaid mills” built around NPI theft often obtain the provider number of a licensed practitioner or practice to exploit that practitioner’s or practice’s billing credentials. Once a Medicaid mill has an NPI, it will appear that the NPI holder is submitting fraudulent claims, regardless of actual complicity.
In California, the Los Angeles County Department of Mental Health appeared to bill Medicaid on behalf of Healthsmart Pacific, a currently defunct hospital in Long Beach that has been banned from receiving federal reimbursements since April 2021, for more than $1.6 million for services rendered between May 2021 and February 2024.
BOGUS BUSINESSES AND ‘LAX’ OVERSIGHT: HOW HOSPICE FRAUD HAS FLOURISHED IN CALIFORNIA
The former chief financial officer and the former owner of Healthsmart Pacific, which did business as Pacific Hospital, were federally convicted of orchestrating a sprawling, long-running healthcare fraud conspiracy that involved illegal kickbacks paid to dozens of orthopedic surgeons and chiropractors in exchange for patient referrals.
A federal investigation, dubbed “Operational Spinal Cap,” into the 15-year kickback scheme at Pacific Hospital found that thousands of patients were referred for spinal surgery by physicians bribed into performing the procedure on them.
Kickbacks to the compromised doctors were financed mainly by money generated from the sale of medical devices surgically implanted into the patients, who were all injured workers. The scam had exploited a heavily abused “pass-through” California law that let hospitals pass on to the state workers’ compensation insurance system the full cost of medical devices implanted in spinal surgery patients.
Pacific Hospital’s owner, Michael Drobot, had also owned a medical hardware company called International Implants, through which he tacked on an additional $250 per device, knowing that the legislation’s provision would require the state to pay the full amount of the invoices. Overall, the racket generated almost $600 million in fraudulent billings.
As for the more recent Medicaid claims, it is unclear whether Healthsmart Pacific treated only the Medicaid recipients or whether they simply did not receive the related reimbursements.
Excluded entities are explicitly prohibited from farming out their billing services so that claims are submitted indirectly through another party. Prohibited providers may treat Medicaid patients on a private-pay basis; those services will just not be reimbursed by Medicaid.
The Washington Examiner contacted the county’s DMH about the nature of its billing relationship with Healthsmart Pacific, whether it is aware of Medicaid claims submitted in its name, and, if so, whether the department billed solely while the hospital performed the billable services.
Los Angeles County DMH was the second-highest billing provider from fiscal 2019 to 2023, with 23.5 million claims totaling $4.7 million in Medicaid funds.
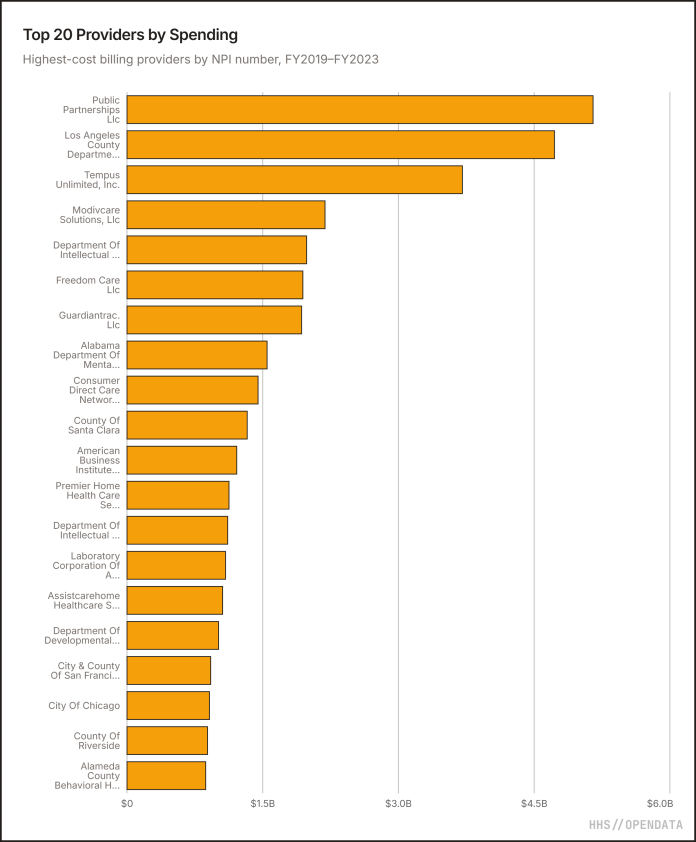
Ten of the 20 top “providers” by spending were state or local agencies that both administer and deliver Medicaid benefits. Aside from Los Angeles County’s mental health department, the biggest Medicaid billers included the city of Chicago, the Alabama Department of Mental Health, and San Francisco’s combined city and county government, the only consolidated city-county in California.
According to a brief from KFF, a health policy research organization, how jurisdictions deliver Medicaid benefits varies widely, but health departments often pay providers to deliver specialized services or treat patients directly, particularly for patients with behavioral health needs and developmental disabilities.
